Health care spending in the United States is increasing faster than the gross domestic product. This trend is obviously neither preferable nor sustainable. And all players are on board for solutions. All players also want a system in which consumers receive the best available options for care, one that prioritizes growth and innovation. Enter the Institute for Clinical and Economic Review (ICER) which helps to determine which are truly value based treatments.
Founded in 2006, ICER is an independent and non-partisan research organization that evaluates the clinical and economic value of prescription drugs, medical tests, and other health care products. The topic resists such simple reduction, but for those who are launching products that can save lives and vastly affect real-time quality of life, ICER, or incremental cost-effectiveness ratio, requires a thorough understanding.
What is ICER?
The Institute for Clinical and Economic Review was established 13 years ago, and today it receives major funding from a private foundation and additional funding from private insurers. ICER methodology uses economic analysis to recommend a price at which an innovative drug provides market value. It also estimates whether a new drug or device is a better value than the next-best and currently available option.
Health care costs are a concern. So are innovations that save human lives. In short, ICER affects whether innovations in care will reach patients by determining whether they meet the ICER-established value-based price benchmark and, accordingly, whether insurance will pay for them.
“Value-based” in healthcare can mean many things
The term “value-based” is like “I’ll call you later.” It has multiple meanings. ICER describes its methodology in terms of analysis of a product’s medical efficacy and its economic value. The latter is assessed by how it affects long-term treatment outcomes. Put another way, it’s two-step process works like this.
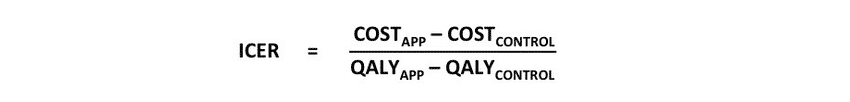
The first stage establishes care value, or how an innovation measures up to an existing and cheaper alternative, and its monetary cost per quality-adjusted life year, or QALY.
The second stage of an ICER evaluation determines an innovation’s health systems value, which consists of the methodology’s judgment of whether it is affordable for health plans. The second stage culminates in a recommended cap on the price of new drugs.
Such a price cap is intended to slow pharmaceutical spending to a rate slower than the gross domestic product. This is important, and the potential fallout for medical advancement and vulnerable patients is also real.
The life science industry’s perspective on ICER
The way the industry views ICER depends on who you ask. ICER benefits private health insurance companies. It also benefits Medicare, the nation’s largest health insurer that by law cannot negotiate with pharmaceutical companies. A 2015 Boston Globe article shares statements of support from health insurance companies and concern from big pharma regarding obscurities in methodology, impact on innovation and the effect both can have on vulnerable patient populations.
Older adults: Too expensive?
A report from the Alliance for Aging Research summarizes some demographics whose lives ICER reports could negatively affect. This includes those with disabilities, veterans, patients with rarer and more complex medical conditions and older adults. Further, it discusses whether the use of QALYs and similar evaluations for treatment and reimbursement constitutes discrimination under federal law.
What comes next for ICER?
ICER affects innovation and access. The cost of health care is high. So is the cost of isolating people from the best quality care available to them.
Snowfish partners with leaders in the life science industry to help navigate the complex market landscapes for multiple conditions and allowing for more effective decisions. Learn more at Snowfish or reach out to us at info@snowfish.net.
- Market Access: The Latest Hurdle for Treating Alzheimer’s and Dementia - June 14, 2023
- Rare Disease Outreach a Missed Opportunity - November 7, 2022
- So You Read Our Previous Post on Biomarkers? - August 1, 2022



